Posted by: Philadelphia Eye Associates in Eye Health on May 6, 2026
Written by Ommay Farah and Raia Francisco, edited by Brad Feldman, MD.
Age-related Macular Degeneration (AMD) is an eye disease that affects 1 in 10 Americans over the age of 50 and is the third leading cause of blindness globally1,2. AMD is a condition in which the central portion of the retina, the macula, starts to degenerate over time. The light signals gathered by the macula are transformed into visual images by a region of the brain called the primary visual cortex.
The macula, a specialized portion of our retina, contains a high concentration of cone photoreceptors and is responsible for our central, color, and detailed vision.
The development of macular drusen, which are protein and fat deposits under the retina, is associated with early signs of the thinning and drying of the macula. These drusen can cause symptoms such as fading of color vision, a blank spot in central vision, blurring of vision, or metamorphopsia, which is the bending or warping of vision.
Potential genetic factors involved in the development of AMD were identified by Genome-Wide Association Studies. These studies indicate 60 genes that may be implicated in individuals who develop AMD3.
In addition to genetic factors, lifestyle factors are also involved in the development of AMD. These factors include smoking4, obesity5, high blood pressure6, exposure to UV radiation8, and high cholesterol7.
AMD is classified as either non-exudative or exudative. Exudation is the process by which fluids and cells are released from blood vessels, which is why exudative AMD is referred to as ‘wet’ AMD, whereas non-exudative AMD is referred to as ‘dry’ AMD.
Dry AMD is subdivided into early, intermediate, and late stages, characterized by the presence and accumulation of macular drusen. Dry AMD is monitored closely by annual or semi-annual ophthalmology exams, and patients are told to come in for additional examinations should they notice any changes in vision.
About 10 percent of individuals with dry AMD eventually progress to wet AMD, which is associated with the development of choroidal neovascularization. This means that new abnormal blood vessels form causing swelling, fibrosis, and bleeding in the macula. If left untreated, wet AMD can lead to irreversible vision loss.
AMD can be diagnosed by analyzing an individual’s retina with a machine called Optical Coherence Tomography (OCT). The machine is used to see cross-sectional images of the retina, which is then used to evaluate the health of the macula, identify any signs of drusen, grade AMD, and track its progression. The images obtained by the OCT can also detect swelling caused by wet AMD.
AMD is often managed by routine eye exams, use of an Amsler Grid, eye vitamins, and Anti-VEGF injections. Routine eye exams and Amsler grid self-exams are used when a patient presents with dry AMD. The Amsler grid is a black and white grid that appears differently to patients depending on the progression of their AMD. As a patient develops additional macular drusen or new blood vessels form, the straight lines on the grid can appear wavy, blurred, faded, or missing.
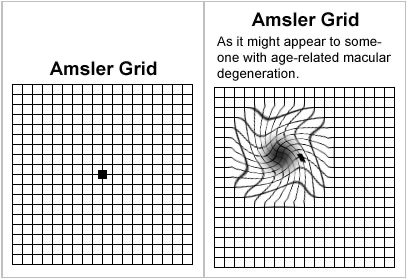
What the Amsler Grid might look like for someone with AMD
Physicians recommend PreserVision AREDS 2 Formula Eye Vitamins for individuals with wet or late-stage dry AMD because of research conducted by the NIH-funded National Eye Institute9. Patients who have developed wet AMD are also treated with Anti-VEGF injections.
VEGF stands for Vascular Endothelial Growth Factor, which comprises a set of signaling proteins that lead to new blood vessels. The excessive activity of these VEGF molecules is the cause of the neovascularization present in Wet AMD, and the effects of these proteins can be countered with Anti-VEGF injections.
Anti-VEGF injections come in various formulations, though they all serve the function of binding to VEGF proteins, leading to blocking the formation of abnormal blood vessels. Anti-VEGF injections can reduce the leakage and swelling of the vessels, ultimately leading to improvement in the vision. These injection treatments, administered by retina specialists, require consistent treatment, varying from six to eight weeks depending on the patient’s condition and tolerance.
If you have a family history of AMD, experience any symptoms, or are concerned about the risk of developing AMD, please schedule an appointment and see your ophthalmologist.
__________
8025 Roosevelt Blvd.
Philadelphia, PA 19152